Wellness programs. HDHPs. EAPs. These phrases have been known to court dread and annoyance in equal measure – but in the modern healthcare world, employers can’t afford to turn their employees off to these options anymore.
As employers continue their shift away from the patriarchal (and expensive) benefits system of the past, most by now have realized that they have to put the ball in the employee’s court. But without the right guidance and communication, employees become frustrated with their new, supposed individuality and either stick to the old system or – at worst – find another place to work.
Luckily, enough time has passed that a combination of true innovation and thorough studies have been done to better help employers become advocates for their employees, rather than annoying (or even suspicious) father-figures. Employers now have plenty of options to help employees personalize their benefits options as well as improve their engagement in the services that are meant to help them.
HR Dive spoke to a number of experts in the field and listened in at panels at the National Business Group on Health Business Health Agenda conference to figure out how to improve employee health (and the bottom line) without losing engagement.
Overwhelmed by choice: Using HDHPs
While more options can help employees personalize benefits to their needs, employees are currently "overwhelmed" by choice. According to a presentation at the National Business Group on Health conference in D.C. last week, 47% of consumers don't know what health services cost and 75% don't fully understand their benefits.
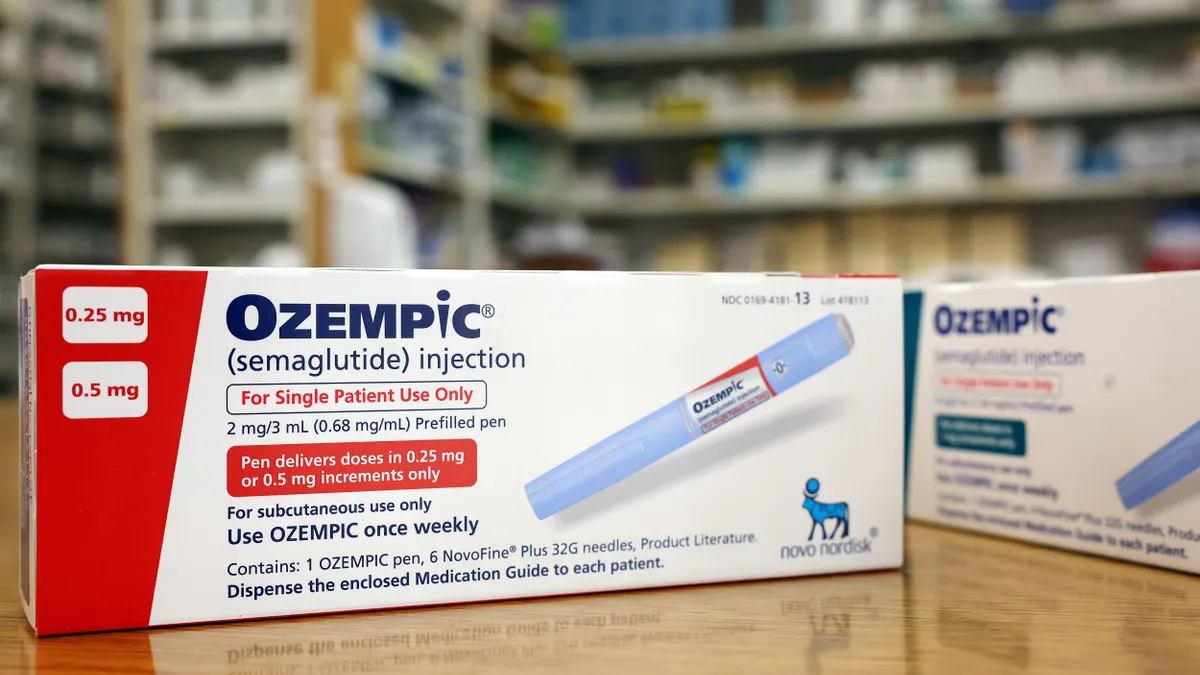
Those stats may explain why high deductible health plans are seeing increased adoption but lower satisfaction. Benefitfocus released its State of Employee Benefits report that revealed 41% of employees on its platform chose an HDHP over other plan options, the report notes. But the Consumer Health Mindset study by Aon Hewitt, The Futures Company, and the NBGH reveals that only 59% of consumers surveyed who are enrolled in an HDHP said they were satisfied with their current plan, versus 76% overall.
"Generally, HDHPs are more work," Joann Hall Swenson, a partner at Aon Hewitt, told HR Dive. "They may be cheaper from a premium perspective, but employees must be more conscientious and that takes more work."
However, Jeff Oldham, VP of Voluntary Benefits Strategy at Benefitfocus, said that their data (directly pulled from thousands of employees on their platform alone) didn't reflect such a trend. While he said it may be true that those on HDHPs may be more likely to experience "buyer's remorse," he also said that employees that used their tool were able to project their potential healthcare spend, and therefore better able to see if an HDHP would be a good fit.
Voluntary benefits, such as accident coverage and critical illness coverage, as well as HSA and FSA funds are all ways for employees to protect themselves financially while on an HDHP – but either employers don't offer them or employees don't utilize them. Only 36% of large employers on the Benefitfocus platform offer at least one of these "gap products," but only 14% of employees are actually enrolled in them, the report revealed. Large employers need to do a better job of "illustrating the value" of the voluntary products so their employees on HDHPs will take advantage of them.
"Employers have to communicate the heck out of it during open enrollment," he said of HDHPs. "You really have to communicate. It's gotta be this perpetual, ongoing month by month communication."
Aon's data agrees. Employees desire "clearer and simpler" communication that is "less enrollment-focused," according to their report. They generally desire communication that is streamlined and personalized, Swenson said.
"The communication was really bad before. People didn't understand them," Oldham said. "But in this new consumer healthcare world, we found new meaning in these products."
Decision support: Powerful new technology
The sector perhaps most helping employees redefine their benefits experience: HR technology.
In the not-so-distant past, decision support tech was fairly one-size-fits-all, Scot Marcotte, client technology leader for Xerox HR services, said. Now, employers must ensure communication with employees is fitted to each employee's needs and preferences.
Texting, for example, has made its way into the benefits communication space. 15% of employers said they were planning to implement it in their communications options next year, and 40% were planning to implement in 2-3 years. To reflect the growing desire for personalized, trusted communication from benefits sponsors, many vendors are turning toward texting as one way to get messages across.
But employers will have to serve as arbiters, choosing which vendors will be allowed personal access to their employees, Marcotte said. Allowing opt-in is also critical, he added, especially since apps that have push notifications have also made a strong appearance. Karen Marlo, vice president of the NBGH, added that the tech has reached such levels of personalization that it can target certain audiences experiencing particular health issues or events, and send push notifications when it notices a trend.
More generally, wellness and EAP programs tend to see more success when employers rebrand them as "life" programs, Marlo added, especially as more employees seek work-life balance.
"You have to be a true advocate for the individual," Marcotte said. "You have to be that advocate in an informed way, and help coach them."
Making it convenient: Onsite Clinics
One way that employers have been moving away from a strictly patriarchal relationship and into a role as an advocate: onsite clinics.
Cindy Pulido, Benefits leader at Facebook, and Scott Shreeve, CEO of Crossover Health, both spoke on a panel at the NBGH conference about how Facebook has implemented an onsite clinic program that provides convenience to employees and encourages them to keep better tabs on their health.
It's not Silicon Valley opulence. The program has saved Facebook money on a number of services, including 44% lower prescription spend per patient as well as 28% lower medical spend overall, Pulido said during her presentation.
The services are open for employees to try for any malady. Their program at Facebook has 80% engagement thanks to what Scott calls a mix of branding, design, delivery model and technology. Above all, he thinks the program encourages employees to act and feel more accountable for their health.
Such an option tends to be "laissez faire" in nature, Shreeve said, thus shirking the patriarchal, authoritative attitude toward benefits of old. Employees are free to use the program or not – Facebook simply provides the convenience and choses not to incentivize the program. (Other companies on the panel, including Cerner, did incentivize their clinic and pharmacy programs).
"It's not about visits, but about providing what patients need in their journey," Shreeve said.
Notably, such clinics require heavy upfront investment, and don't fit employers that have less than 2,500 employees in one spot. But Scott notes that the reasons for adopting an onsite clinic vary from purely financial reasons to culture differentiation. Facebook wanted to "provide great quality of life" for their employees.
"Employers are saying, this is a part of the health chain I can't control," Shreeve said. Encouraging employees to see the appropriate health care professional in a timely manner (aka not going to the ER for the wrong reasons) is often only done via some sort of education initiative, if that. Bringing healthcare providers directly to campus is convenient and controlled.
Such programs are a newer form of innovation for employers that want to give employees more individual control over their healthcare while also managing their costs in an effective way.
"Whatever the solution, it has to get to the heart of what people want to engage with," Shreeve said.
And at the end of the day, that's what matters.