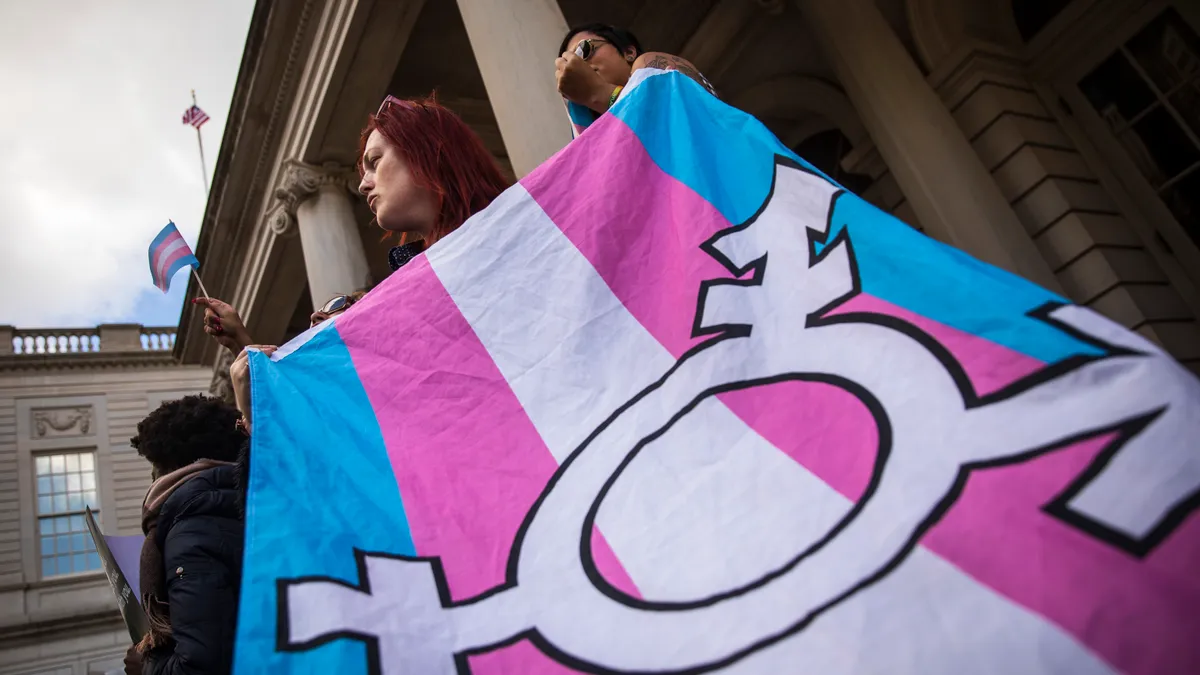Dive Brief:
- Because the North Carolina State Health Plan receives federal funds, it is not immune from a suit from state employees saying it violated the Affordable Care Act when it excluded gender-confirming health services, the 4th U.S. Circuit Court of Appeals ruled (Kadel, et al. v. North Carolina State Health Plan for Teachers and Employees, et al., No. 20-1409 (4th Cir., Sept. 1, 2021)).
- North Carolina removed an exclusion for gender-confirming care for its 2017 health plans and allowed the services "to be reviewed under the same criteria and in the same manner as claims for any other medical, mental health, or pharmacy benefits." But a new state treasurer took office in 2017 and saw to the reinstatement of the plan's exclusion, pledging that the policy would remain until courts, lawmakers or voters required him "to spend taxpayers' money on sex change operations."
- Plaintiffs argued that the plan discriminated against transgender enrollees by categorically denying coverage for treatments related to gender dysphoria such as counseling, hormone therapy and surgery. Such a denial violated the ACA, they said, and the workers sought monetary damages and equitable relief. A district court denied the health plan's motion to dismiss the claims — a decision the 4th Circuit affirmed. The health plan gave up its immunity against the workers' allegations when it accepted federal assistance, the court argued, so it must face the suit.
Dive Insight:
When organizations face issues related to employing transgender individuals, they are generally considering concerns related to Title VII of the Civil Rights Act of 1964, rather than the ACA, the law the 4th Circuit considered here. Title VII claims arise frequently; the law's protections were recently expanded by the U.S. Supreme Court to include a prohibition against discrimination based on gender identity and sexual orientation.
When the High Court handed down its ruling, however, it left several questions unanswered. One such question had to do with healthcare — would Title VII require employers to make changes to their employee benefit plans?
Courts have been weighing in. An Illinois district court, for example, applied the Supreme Court's Bostock analysis to rule for an employee who alleged her union engaged in sex discrimination when it refused to enroll her wife in health insurance it previously granted only to heterosexual couples.
"There can no longer be any dispute that the conduct alleged constitutes sex discrimination," the court noted. "Had [the worker] been a man seeking spousal coverage for a wife, coverage would not have been denied. She did not receive this coverage because she was a woman seeking coverage for her wife."