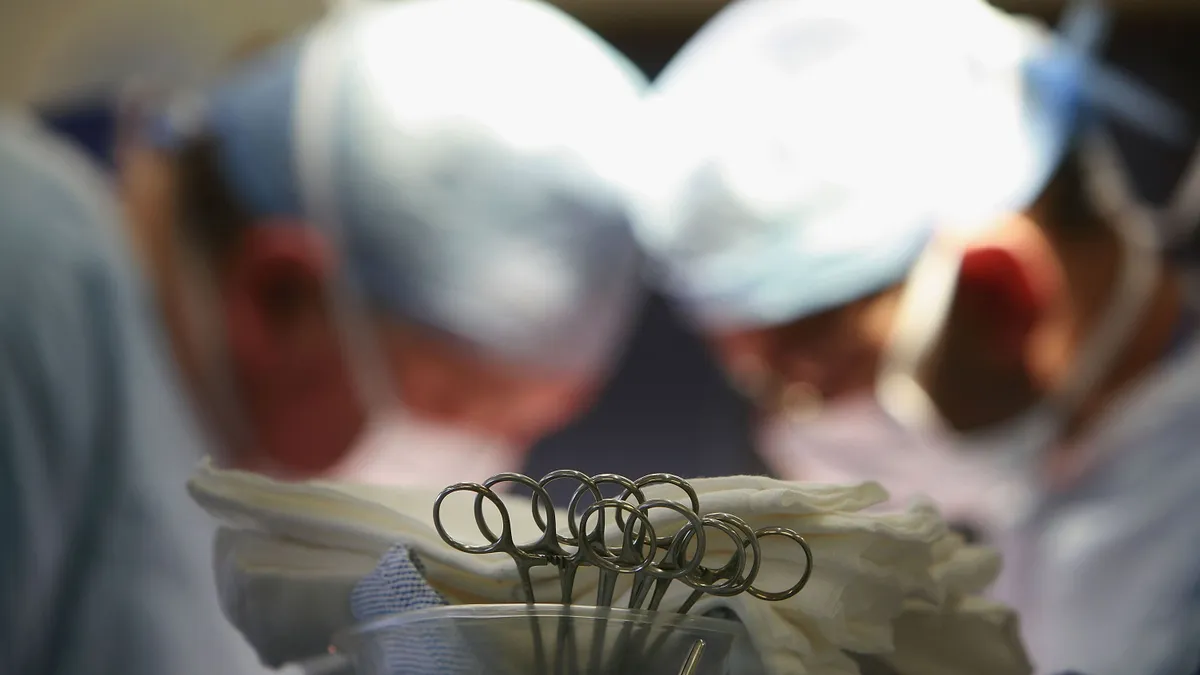
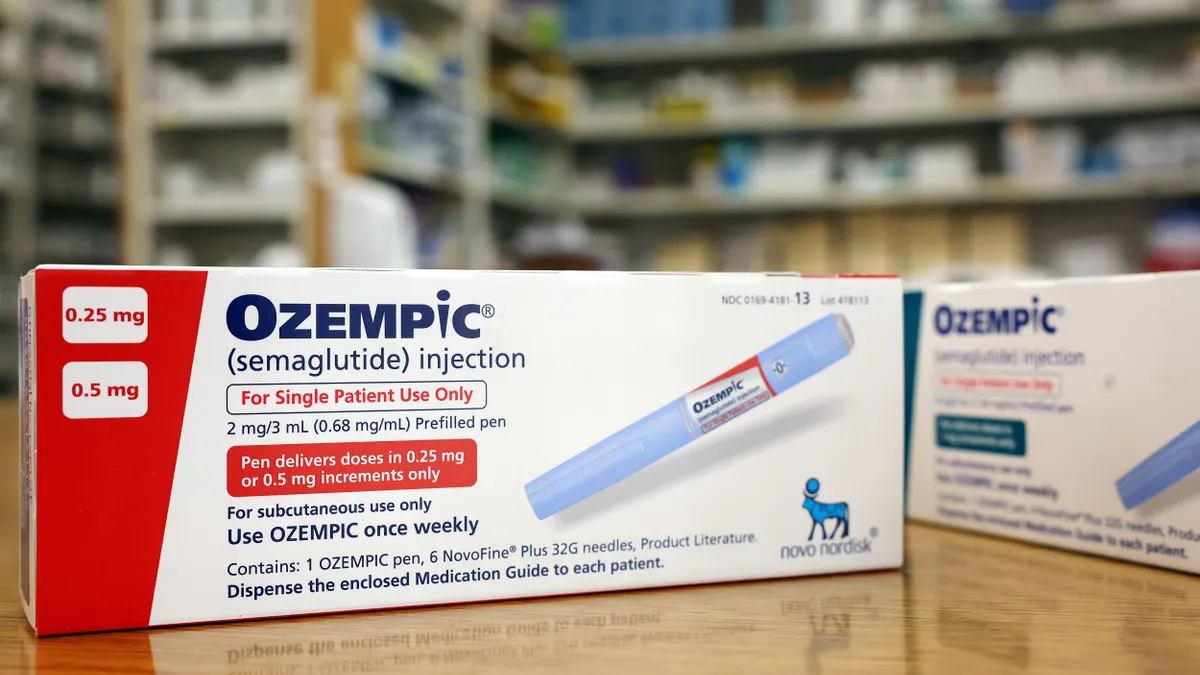
Pharmaceutical pricing controversies create easy headlines. But issues with EpiPen prices and HIV drug availability reflect the conundrums employers face with specialty pharmacy: some employees need these expensive drugs to function…and someone (usually, ultimately, the employer) has to pay for them.
In the NBGH Large Employers’ 2017 Health Plan Design Survey, specialty pharmacy was considered the No. 1 driver of medical trend for the first time. Three years ago, it wasn’t even in the top five, Brian Marcotte, president and CEO of the NBGH, said.
So why is this concern growing now?
HR Dive spoke to experts in the field to get a sense for what’s triggering this anxiety, and what employers are doing – and will soon be able to do – to keep costs under control.
Why now?
Part of the concern seems tied directly to increased awareness of cost issues in general, Susan Garfield, a principal in EY’s Life Sciences Advisory practice, told HR Dive. Several years ago, employers began looking at hospital costs, managing care pathways more aggressively, and the like.
“It’s partly the natural profession as the entire healthcare continuum started addressing those other costs,” Garfield said.
Both Garfield and John Jaeger of Decision Resources Group provided a few reasons why the concern reached such a heightened level now:
- Quite simply, pharmaceutical pricing has garnered strong public attention in the past year thanks to controversies such as the aforementioned EpiPen pricing issue and the Martin Shkreli pricing scandal. It’s entered the presidential campaign discussion, Jaeger noted, and for many, creates an “easy story line,” Garfield added. But as the media storm continues, the complexity of pricing tends to get lost – meaning patients are angry but not quite sure what can be done.
- An “enormous amount” of innovation has also taken place in the biopharma market, Garfield said. With innovation comes the promise of new types of specialty medicine, such as personalized pharma – but such products, as incredible as they may be, are also perceived to have high price points. Employers are beginning to prepare for that reality now.
- Employee populations are aging. People are working beyond the traditional retirement timeframe, so “larger populations of employees with expensive issues are increasing,” Garfield noted. On top of that, employers play a larger role than ever in arranging employee access to treatments, managing burden of cost and providing quality of life.
CDHPs: Bridging the knowledge gap
One large difference between now and five years ago: More patients are acutely aware of the price of specialty drugs thanks largely to high-deductible health plans. In essence, employers are beginning to see the limits of benefit design changes, especially as employees pay more money out of pocket, Jaeger noted.
“Much of the angst around the EpiPen was driven by the level of cost exposure that many families found themselves within CDHP plans,” Jaeger said. “Patients are finally getting a true look at the cost of drugs and the market is pushing back.”
Ten years ago, most employees were still on traditional plans that shielded them from the vagaries of expense, Jeff Oldham, Vice President of Consumer Strategy at Benefitfocus told HR Dive. The cost burden is now widely shared between employer and employee, instead of being entirely the area of the employer – good for the employer, but trouble when employees aren’t receiving the quality care they need due to expense.
The most popular solutions to solve pharma problems continue to be specialty pharmacies and utilization management – the top two current techniques of employers polled by the NBGH. Specialty pharmacies are specifically set up to take care of patients with expensive, complicated drugs by providing education, 24-hour access, continuous communication and management, and financial assistance. In general, high-touch solutions that keep both employees and employers informed as they deal with new cost burdens seem to top the list of favored management techniques.
Emerging alternatives
Thanks to new pharma technology, some employers are looking toward therapeutic alternatives to cover some rising costs. "Therapeutic alternatives" is a general term that sometimes includes generics – but in the case of specialty pharmaceuticals, there often is no generic option.
Instead, biosimilars have garnered attention from employers. These drug types take up an interesting niche in pharma markets. While generics tend to be seen as the same or exchangeable for a branded product, biosimilars are (as their name suggests) seen as similar, but not 100% equivalent, Garfield said.
Obviously, a biosimilar may not work for every patient – and it may not exist for certain medications yet, making for a potentially “complex road” for employers. But they are already impacting the market in positive ways. When a biosimilar enters the market, it tends to have an “impressive effect” on brand prices, Garfield said.
“It has an aggregate impact on brand price points, which decreases overall cost of care when a biosimilar enters,” she added. Essentially: therapeutic alternatives are good for employers because they create pressure in the market to provide cost-effective treatments that generally push prices down.
In the past, employers were presented with coverage options and cost and looked at access in terms of formulary tiers, budget impacts and similar levers. The real future for employers, Garfield said, is the opportunity to be more involved on the other end of the process.
“I think employers in the future will have the opportunity to be participants in the delivery paradigm,” she said. Especially around chronic disease, employers could be part of an innovative program that involves them at multiple levels of care to ensure the best outcomes for their employees.