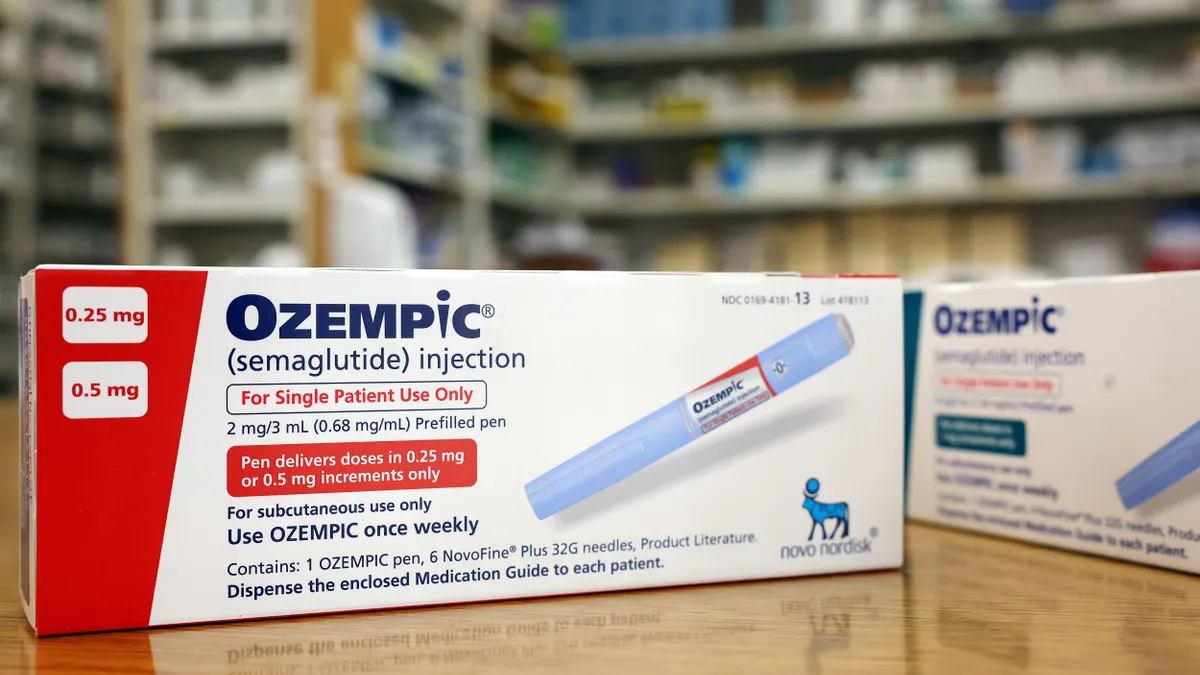
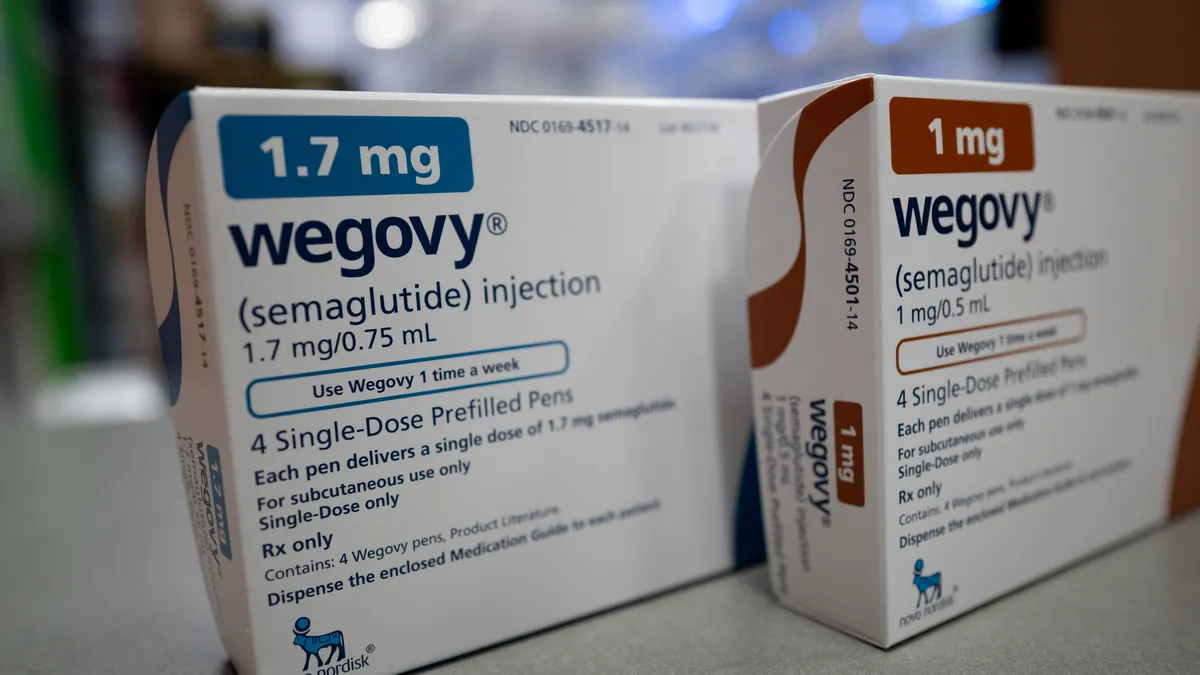
With the omicron variant's spread and case numbers on the rise, there's no doubt the pandemic continues. The same can't be said, however, of the provisions legislators enacted to help American workers maximize their benefits to cope with the global health crisis.
"There's very little that was enacted as a result of the pandemic that continues," said Jody Dietel, senior vice president of advocacy and government affairs at HealthEquity.
Several benefits-related elements of the Coronavirus Aid, Relief, and Economic Security Act and the American Rescue Plan Act are set to expire at year's end. Congress would have to act quickly to retain the measures they introduced at the start of the pandemic, Dietel told HR Dive in an interview.
The changes may disappoint employers and employees. "A lot of these provisions really made a lot of sense," Dietel said. "We just haven't been able to get the attention of Congress."
Unless Congress jumps into action, these five provisions will fade at year's end:
1. CARES' safe harbor provision
Employers and employees will say goodbye to the CARES Act's "safe harbor" provision in the new year. The provision allowed high-deductible health plans to cover telehealth and other expenses from remote care services before individuals met their deductible.
2. CARES' flexibility for FSAs
Before the pandemic, employees' elections toward their flexible spending accounts were irrevocable. The CARES Act changed that, allowing workers to change their elections at any time, for any reason.
"That was a very flexible rule, and it helped people because there was so much uncertainty," Dietel said. "It was a very common-sense flexibility provision from Congress. They did a great job."
3. ARPA's higher dependent care contributions
ARPA boosted the maximum amount of money employees could set aside for dependent care, raising the top limit from $5,000 to $10,500. Congress also allowed employees to change their dependent care reimbursement account elections mid-year, so that employees could select higher limits.
If Congress doesn't extend ARPA's higher exclusion limit, elections for dependent care reimbursements will be limited to $5,000, plus any unused dependent care reimbursement account funds from 2021.
4. ARPA's six-month COBRA subsidy
It may be easy to say goodbye to ARPA's COBRA subsidy. "It's too bad that it took so long to work on this, and that it was so difficult to use," Dietel said. "It didn't help some of the people it was supposed to help."
The CARES Act allowed workers to get unemployment if they couldn't risk exposing cohabitants to the virus by clocking into work. But legislators didn't apply that philosophy to ARPA's COBRA subsidy. To qualify, workers had to be terminated involuntarily.
5. Consolidated Appropriations Act's unlimited carryovers
The Consolidated Appropriations Act allowed for unlimited carryovers stemming from contributions made to DCRAs and FSAs for the 2020 and 2021 plan years. "At the end of this year, if your employer adopted those provisions and you have something left, it can carry over," Dietel said. "At the end of next year, it goes back to the statutory requirements."
Without congressional action, those statutory requirements make no room for carryovers of funds designated toward dependent care. For healthcare, carryovers are limited to 20% of the statutory contribution limit, which is $570 for next year.
The act also extended the grace period that gave individuals more time to spend the money they set aside. Prior to the pandemic, that grace period lasted two and a half months. The act extended that time to one year. "If I had any money left from 2020, I could use it any time in 2021," Dietel explained. "That provision applied to both healthcare and dependent care. But both of those extensions expire at the end of this year."
What won't change?
There are two lasting holdovers from the coronavirus legislation:
- The IRS will continue to view the purchase of hand sanitizer and face masks to prevent the spread of COVID-19 as eligible medical expenses and allow for reimbursement. Neither of these items meets the traditional definition of an eligible medical expense, Dietel pointed out. (The purchase of face masks and hand sanitizer to prevent flu and cold is not eligible, Dietel noted.)
- Under the CARES Act, individuals will no longer need a prescription to receive a reimbursement for over-the-counter drugs.
What do these changes mean for HR pros?
While vendors will implement the changes, HR pros will likely need to take charge of communication, Dietel said.
"They should encourage employees to look at their expenses to ensure they're taking advantage of the tax vehicles they can," she said. HR pros need to be available to help employees review their choices and select the best options during enrollment.
Those in charge of benefits can target their communications toward employees who took advantage of the pandemic provisions. Dietel suggested HR pros "do some data mining" to find the employees who most need to understand the changes. Employees who took out a $10,500 election for dependent care, for example, need to know they can't do that this year, more so than the worker who didn't bother with any dependent care election.
As HR pros develop a communication campaign, they should consider asking their vendors for help, Dietel said. Most vendors offer tools and resources employers can use to educate workers about their options.
Employers can lean on their vendors for information, too. The fading provisions will likely inspire confusion, and a good vendor will be able to provide reliable information about benefits and the changes happening — or not happening — in Congress, Dietel said.
Dietel encouraged HR providers to check in with their administrative partners to make sure they're on top of the changes. Next year's benefits plans should reflect them. "If you start asking questions [about the provisions] and your vendors aren't sure, that's a bad thing," she said.
"If you're not sure, ask," Dietel said. "There are no stupid questions about benefits."